From “seeing once” to “living it always”: how PIC programs and high-fidelity anatomical simulation are redefining the surgical learning curve.
By Ehab Soltan
HoyLunes – In 21st-century medicine, the traditional training model—based on passive observation and assisted repetition—is reaching its limits. The complexity of minimally invasive techniques and the demand for perfect functional outcomes require a new paradigm. In 2026, surgical excellence no longer depends solely on the surgeon’s pulse; it is the result of a critical triad: biology, biomechanics, and high-fidelity training.
Various studies in medical education have shown that the increasing sophistication of surgery demands more structured and reproducible instruction models. The classic maxim “see one, do one, teach one”, which defined training for decades, is insufficient in an environment where procedures increasingly depend on three-dimensional navigation, precision instrumental coordination, and the integration of digital technologies. In this context, advanced simulation and intensive immersion programs have become strategic pillars of contemporary teaching.
The Imperative of Subspecialization
The era of the generalist surgeon is giving way to that of the ultra-focused specialist. “Clinical immersion” emerges not as a conventional course, but as an ecosystem for real-time knowledge transfer. Programs such as the PIC (Clinical Immersion Program), recently held at the Hospital Vithas Valencia 9 de Octubre, demonstrate that the learning curve can be accelerated through a deep integration of advanced theory and simulated practice.
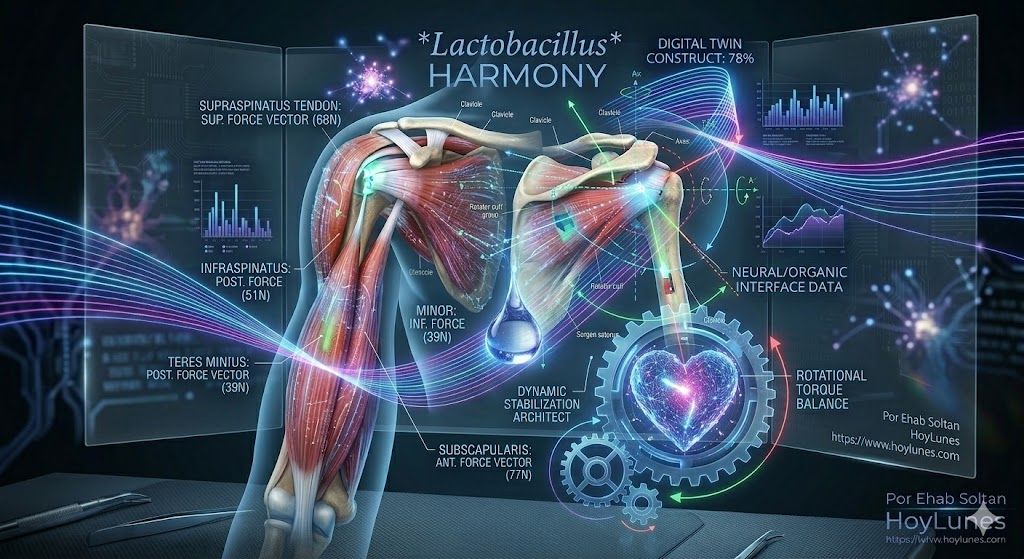
The Success Case: Rotator Cuff Pathology
The shoulder has become the new challenge for functional longevity. With a prevalence ranging between 5% and 40% in the general population—increasing significantly from the age of 50 onwards—the rotator cuff represents one of the leading causes of occupational disability and loss of quality of life.
The increase in life expectancy and the extension of professional activity are amplifying the clinical relevance of these pathologies. In societies with aging and active populations, degenerative shoulder injuries severely limit upper limb function. This trend forces healthcare systems to rethink not only therapeutic strategies but also the formative models necessary to respond to a growing demand for complex procedures.
However, success in this area is not just a matter of suturing. As the program directors, Dr. Juan Aguilar and Dr. José Enrique Aroca, explain, the most critical decision is clinical reasoning: When to intervene and what individualized strategy to apply? Subspecialization allows for discerning which patients benefit from anatomical repair and which require a joint preservation approach.
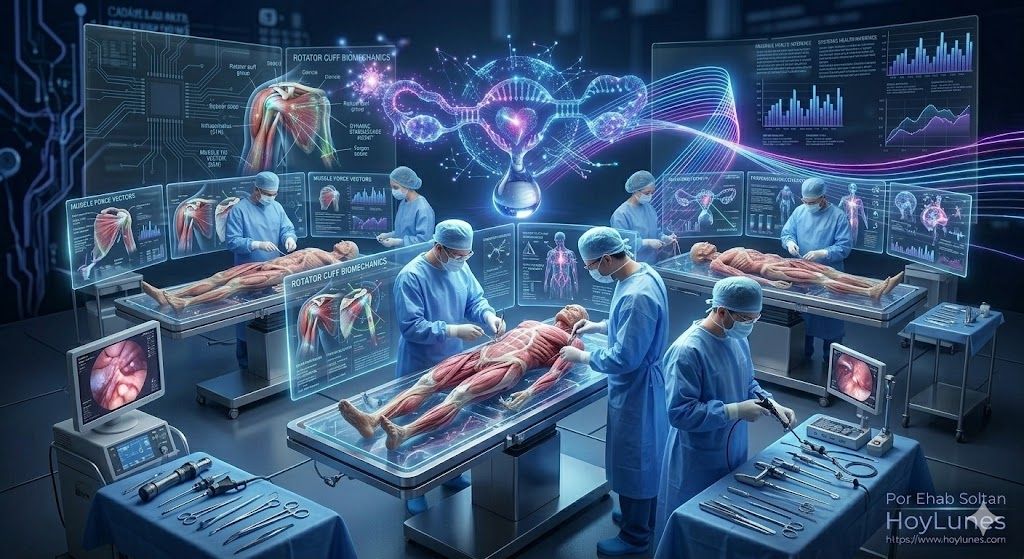
The Three Phases of Total Immersion
For knowledge to be “exceptional,” it must be experienced. The PIC model structures learning into three stages that guarantee the consolidation of competencies:
Phase 1: Live Surgery. Attendees observe preoperative planning and step-by-step technical execution. This is where decision-making under pressure and the resolution of unexpected findings are analyzed.
Phase 2: Anatomical Laboratory Training (Cadaver Lab). In collaboration with the Catholic University of Valencia (UCV), surgeons refine their proprioception on cadaveric specimens. This high-precision controlled environment is vital for mastering navigation in confined joint spaces.
Scientific literature widely supports the value of these high-fidelity simulation environments. Educational studies have shown that repetitive training in anatomical laboratories significantly reduces operative time and improves technical precision when surgeons transition these skills to the real operating room. This model allows for errors to be made in a safe space and converted into structured learning.
Phase 3: Consolidation and Applied Reasoning. The program concludes with a new live surgical session, allowing the concepts practiced in the lab to be re-validated in real clinical situations.
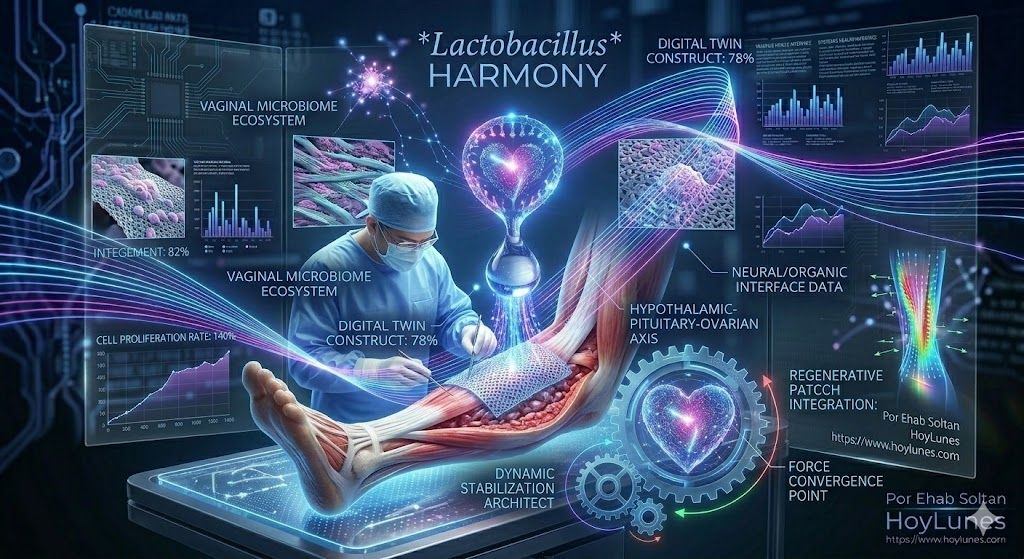
Biology and Technology: The Future of “Biological Augmentation”
Modern surgery at HoyLunes is analyzed through the lens of tissue engineering. It is no longer enough to simply re-anchor a tendon; the goal is to optimize the biological environment to ensure optimal healing.
Biological Augmentation: The use of collagen patches and autologous grafts is revolutionizing success rates in injuries previously considered irreparable.
3D Planning: The integration of three-dimensional models allows for the simulation of joint replacement through shoulder prostheses with mathematical precision, reducing surgical time and tissue trauma.
This approach reflects a broader transition toward the biological optimization of tissue. The integration of biomaterials and engineering strategies seeks to improve both mechanical stability and the quality of the healing process, turning shoulder surgery into a clinical laboratory for regenerative medicine applied to the musculoskeletal system.
Team Stability: The Invisible Factor
An exceptional surgeon is only as good as the team that surrounds them. Clinical immersion underscores that patient safety depends on a shared “culture of excellence”. The cohesion between nursing, scrub technicians, and assistants creates a redundant safety system that minimizes human error and optimizes workflow.
Educational Commitment and the Common Good
The HoyLunes platform recognizes Hospital Vithas Valencia 9 de Octubre as a model of social responsibility. By acting as associate professors and developing advanced programs (such as Dry Lab courses for residents), these centers become engines for public health, raising the national medical standard.
The transformation of surgical education transcends the academic realm. As techniques gain sophistication, formative quality is critical for patient safety and healthcare sustainability. The PIC program illustrates how simulation, structured reasoning, and interdisciplinary collaboration redefine standards of excellence.
Toward a Medicine of Results
Clinical immersion represents the end of improvisation. In 2026, training must be as precise as the intervention itself. By transforming the operating room into a cutting-edge classroom, we are investing in the sustainability of the system and, above all, in the recovery of autonomy for thousands of patients.
Sources and Technical Data
Clinical Direction: Dr. Juan Aguilar and Dr. José Enrique Aroca (Hospital Vithas Valencia 9 de Octubre).
Academic Collaboration: Catholic University of Valencia (UCV).
Area of Analysis: Orthopedic Surgery and Traumatology (Shoulder Unit).
HoyLunes Medical Archive (2026): Simulation systems and the future of surgical education.
#ClinicalImmersion #RotatorCuff #PrecisionTraumatology #Vithas9deOctubre #MedicalTraining #HoyLunes #ShoulderSurgery #EhabSoltan
This is for informational purposes only. For medical advice or diagnosis, consult a professional.



