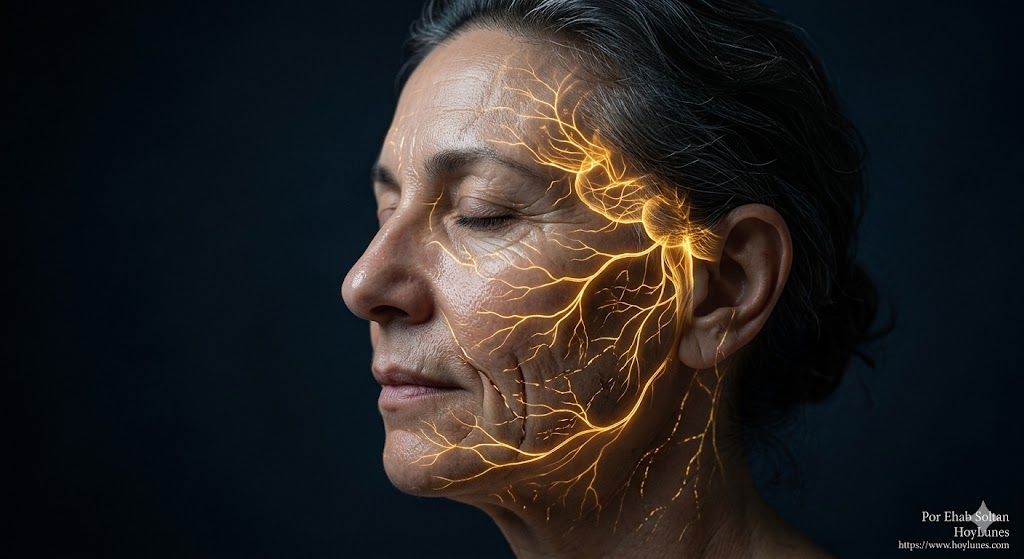
The skin is not just a biological barrier: it is an organ deeply connected to the nervous system, capable of responding to neural signals that regulate inflammation, tissue repair, and cellular regeneration.
New research suggests that visible facial aging may depend not only on collagen or sun damage but also on the way the nervous system communicates and coordinates the skin’s repair processes.
In recent years, various fields—from molecular dermatology to peripheral neurobiology—have begun to explore this connection with unprecedented rigor. Far from being a passive tissue, the skin actively participates in complex signaling networks involving immune cells, inflammatory mediators, and sensory nerve fibers. This interdisciplinary approach is raising fundamental questions about the true mechanisms that regulate cutaneous decline.
By Ehab Soltan
HoyLunes — For decades, we have interpreted the passage of time on the face as a simple sum of external and mechanical factors. Conventional dermatology has built its discourse on three pillars: collagen degradation, the cumulative impact of ultraviolet radiation, and the dictates of genetics.
This explanatory framework has allowed for crucial advances in prevention and treatment, especially in the understanding of photoaging. However, it has also tended to simplify the phenomenon, reducing it to a fundamentally structural process. Contemporary research suggests that this vision, while useful, may be incomplete.
Through a traditional lens, wrinkles are the result of exhausted fibroblasts and an extracellular matrix that loses its supporting capacity; a view of the skin as an architectural material that yields to climate erosion. Nevertheless, in the most advanced biomedical laboratories, a question has begun to emerge that challenges this dogma: What if the visible aging of the skin were also orchestrated by the electrical network that runs through it? What if wrinkles were, in fact, a neurobiological phenomenon?
Formulating this question implies a paradigm shift. It means considering the skin as part of an integrated system where the nervous system, the immune system, and skin cells participate in a constant dialogue that determines the tissue’s ability to repair itself, adapt, and resist chronological progress.
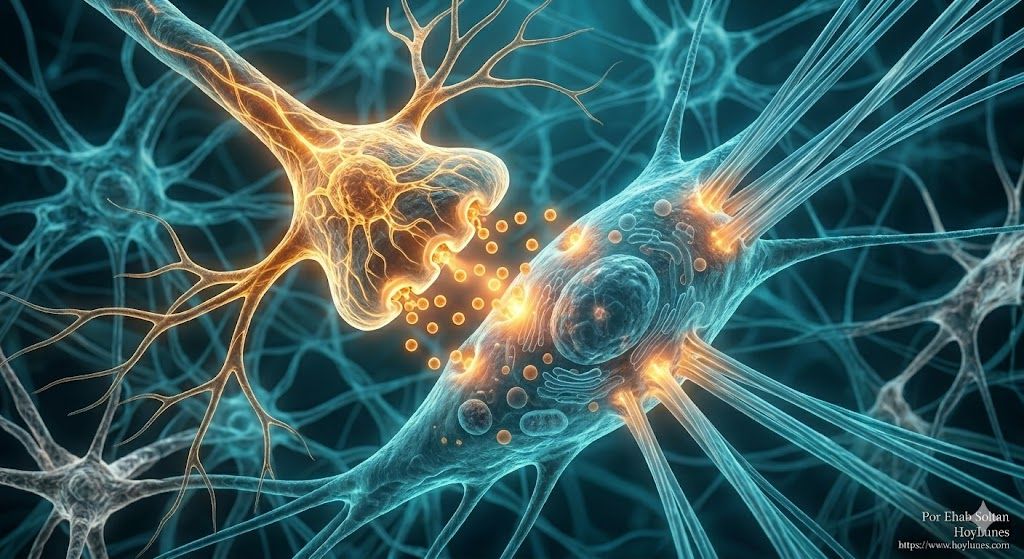
The Skin: One of the Most Innervated Organs in the Body
To understand this hypothesis, we must stop seeing the skin as an “envelope” and start seeing it as an interface. Biologically, it is the most complex bridge between our inner selves and the environment.
Every square centimeter of our dermis is a dense jungle of nerve endings. These fibers do not just detect stimuli; they are active emitters that release neuropeptides and chemical mediators that act as critical instructions for adjacent cells. We are looking at cutaneous neuroimmunology, a field where the nervous system ceases to be a spectator and becomes a primary actor in tissue homeostasis.
This discovery has led the scientific community to describe the skin as a true “neuroimmunological organ”. In this model, nerve signals do not only transmit sensory information but also govern the inflammatory response and cellular repair processes—a concept that has gained indisputable relevance in the most recent studies of cutaneous biology.
The Dialogue Between Nerves and Skin Cells
This molecular dialogue is decisive. Cutaneous nerves have the capacity to modulate inflammation, accelerate healing, and dictate the pace of cellular proliferation. The key interlocutor in this chain is the fibroblast.
Evidence has shown that neural signals directly influence collagen synthesis. When communication is fluid, the skin repairs itself effectively. But if this dialogue is distorted or “neural noise” increases, the balance is broken. The tissue stops receiving precise orders to remain firm, initiating a degradation process that does not emanate from the outside, but from the body’s own command network.
This perspective introduces a vital nuance: instead of interpreting collagen loss solely as a purely passive phenomenon, it is proposed that it could reflect changes in the biological regulation systems that coordinate cellular activity.
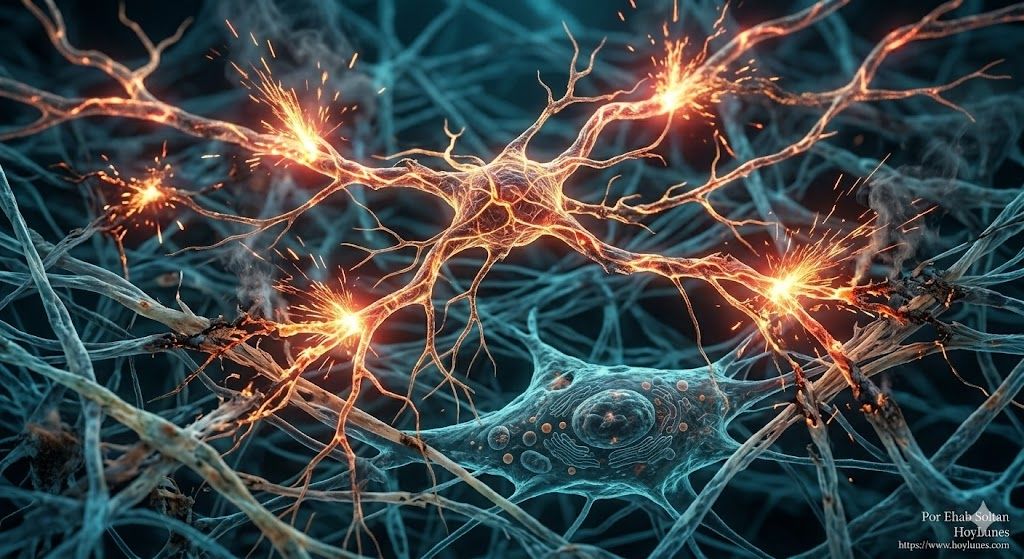
Stress, the Nervous System, and Skin Aging
This is where lifestyle translates into biology. Chronic stress is not just a state of mind; it is a chemical storm that travels through the peripheral nervous system. The prolonged activation of the hormonal axis associated with stress causes a constant release of inflammatory mediators in the dermis.
This phenomenon, sometimes known as inflammaging, accelerates collagen degradation and drains cellular regenerative capacity. The nervous system, under pressure, acts as a central regulator that, instead of protecting cutaneous architecture, accelerates its wear.
Various studies indicate that prolonged stress modifies the activity of multiple neurochemical mediators. Although the exact mechanisms remain under scrutiny, these observations suggest that the psychological and physiological environment influences skin biology much more directly than was estimated just two decades ago.
An Emerging Hypothesis: Neurocutaneous Aging
The final piece of the puzzle is the neurocutaneous hypothesis: the premise that facial aging depends on the functional state of the nerves that innervate it. Like cutaneous tissue, nerves undergo their own process of senescence; they lose precision, and their signaling capacity weakens.
If peripheral nerves can no longer send clear signals to fibroblasts, tissue regeneration becomes erratic. In this light, skin aging transcends dermatology to become a visible manifestation of the decline in neurobiological communication.
In this interpretation, facial aging is understood as a systemic phenomenon. The skin thus becomes an accessible indicator of deep biological processes related to nervous regulation, chronic inflammation, and tissue repair.
What This Idea Would Imply for Aesthetic Medicine
If we accept that the skin ages because the nervous system “stops speaking to it,” the therapeutic paradigm must evolve. Currently, aesthetic medicine focuses mostly on the effect: filling, relaxing, or exfoliating.
This conceptual shift could transform the development of therapies. If nerve signals actively regulate aging, the medicine of the future will incorporate strategies aimed not only at modifying structure but also at influencing the biological systems that control regeneration from its neural origin.
Tomorrow’s approach will seek to restore biological dialogue through:
Signaling Modulators: Formulas that mimic the neuropeptides of young skin.
Neuro-regenerative Therapies: Treatments designed to preserve the health of dermal nerve fibers.
Neuro-cosmetics: Products that interact with the nerve receptors that control cellular function.
Scientific Caution: A Hypothesis Still in Development
Despite the potential of this path, science demands rigor. Understanding the interaction between the nervous, immune, and cutaneous systems is extremely complex. Institutions such as Harvard and the NIH emphasize that we are in an exploratory phase. The neurocutaneous hypothesis is a brilliant promise, a line of research that opens doors, but one that has yet to be consolidated as an absolute clinical truth.
Currently, many of these findings come from cellular models and experimental studies. Translating these observations into clinical practice will require additional research and controlled trials to evaluate their therapeutic efficacy with rigor.
A New Way of Thinking About the Skin
For a century, we have seen the skin as a wall. Today, thanks to neuroscience, we see it as a keyboard. The skin is a dynamic neuroimmunological organ that reacts to our thoughts, our stress, and the integrity of our nerves.
As the border between dermatology, neuroscience, and immunology fades, this interdisciplinary approach offers new keys to understanding how the organism maintains the balance between regeneration and deterioration.
Understanding this connection is the key to a more authentic longevity. The question that prevails is as simple as it is provocative: What if wrinkles were, in part, the visible signal of a profound change in the conversation between our nervous system and our skin?
Scientific Sources and Support:
Harvard Medical School: [https://hms.harvard.edu]
American Academy of Dermatology: [https://www.aad.org]
National Institutes of Health: [https://www.nih.gov]
Nature Publishing Group: [https://www.nature.com]
Journal of Investigative Dermatology: [[https://www.jidonline.org]
This information is for informational purposes only. For medical advice or diagnosis, consult a professional.
#CutaneousNeurobiology #AestheticMedicine #HealthyAging #MedicalInnovation #HoyLunes #EhabSoltan