The systemic connection between asymptomatic dental exfoliation, glycemic dysregulation, and cardiovascular risk: why David’s silence is a medical emergency.
By Ehab Soltan
HoyLunes – Adult tooth loss is rarely an isolated accident or a stroke of bad luck. In the vast majority of cases, it is the final chapter of an inflammatory process that has advanced in the shadows for years. When the body stops sending pain signals, it is not because the problem has vanished, but because the destruction has been so profound that it has disconnected the body’s natural alarms.
The case of David, a 49-year-old patient with Type 2 Diabetes Mellitus and a cardiovascular history, is the perfect example of how the human body attempts to adapt to pathology until it simply gives way.
The Clinical Case: David’s “Expulsion”
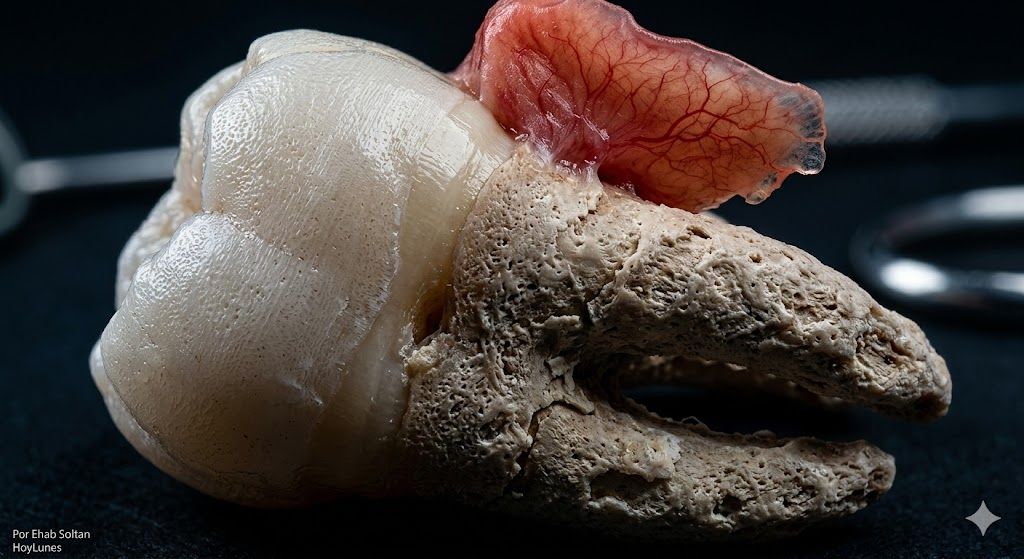
David discovered the fragility of his health on a typical Tuesday while chewing a piece of soft bread. Without any crunching, without hemorrhage, and above all, without that stabbing pain we usually associate with the dentist, his molar detached. In dentistry, this phenomenon is called spontaneous exfoliation.
For David, the absence of pain was a misleading relief. However, for Dr. Arrieta, it was proof of pre-existing pulp necrosis and a massive loss of support. The nerve did not scream because it was no longer there to do so. The differential diagnosis was immediate: we were not looking at trauma, but at the collapse of a structure undermined by years of systemic inflammation.
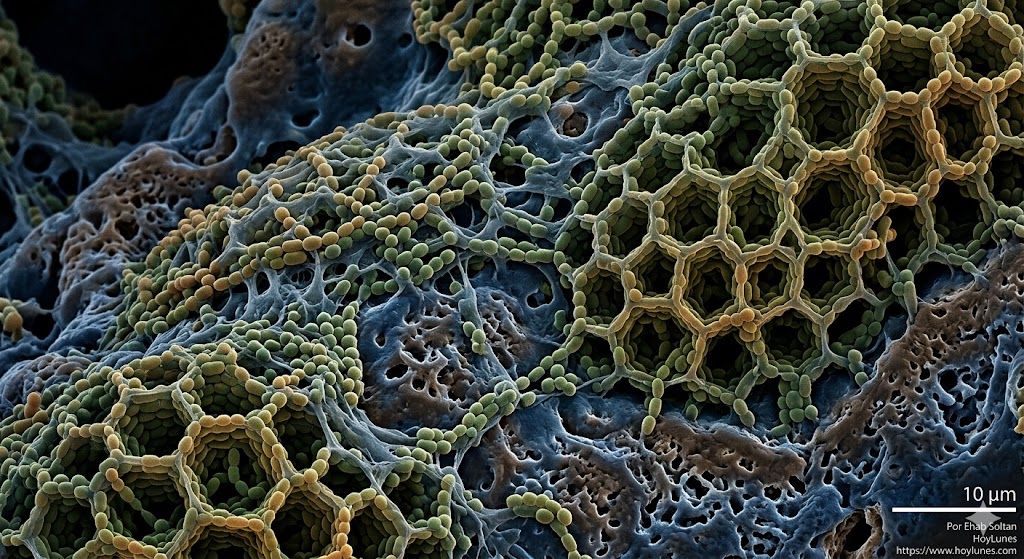
“The absence of pain in tooth loss is not a sign of healing, but evidence that the infection has managed to neutralize the body’s biological alarms”.
Forensic Analysis: Total Loss or Fracture?
Understanding which part of the tooth David lost is vital for determining the risk of generalized infection.
A. Avulsion or Absolute Exfoliation
This occurs when the tooth detaches whole, root included. In adults, this is usually the result of Structurally Advanced Periodontitis. Here, opportunistic bacteria such as Porphyromonas gingivalis do not just attack the gums; they literally “dissolve” the periodontal ligament and the alveolar bone that anchors the tooth to the skull.
The hidden danger: Once the anchorage is lost, the mouth ceases to be a barrier and becomes a highway for inflammatory mediators traveling directly to the heart.
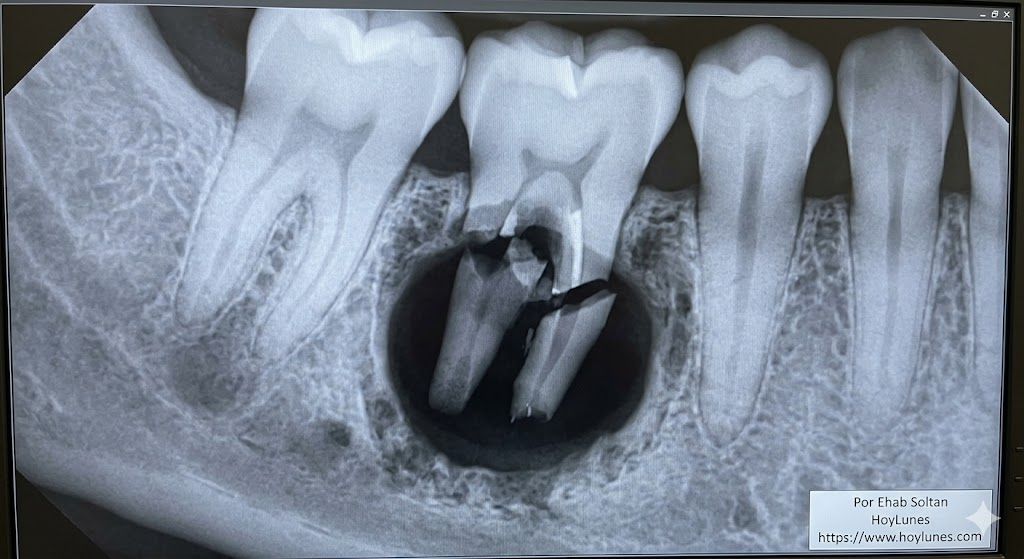
B. Root Fracture (The Buried Threat)
If the tooth breaks and the root—the “root remnant“—remains under the gum, the scenario turns darker. That necrotic root acts as a constant infectious focus. In immunocompromised patients, this “residue” can lead to deep cysts or even facial cellulitis requiring hospitalization.
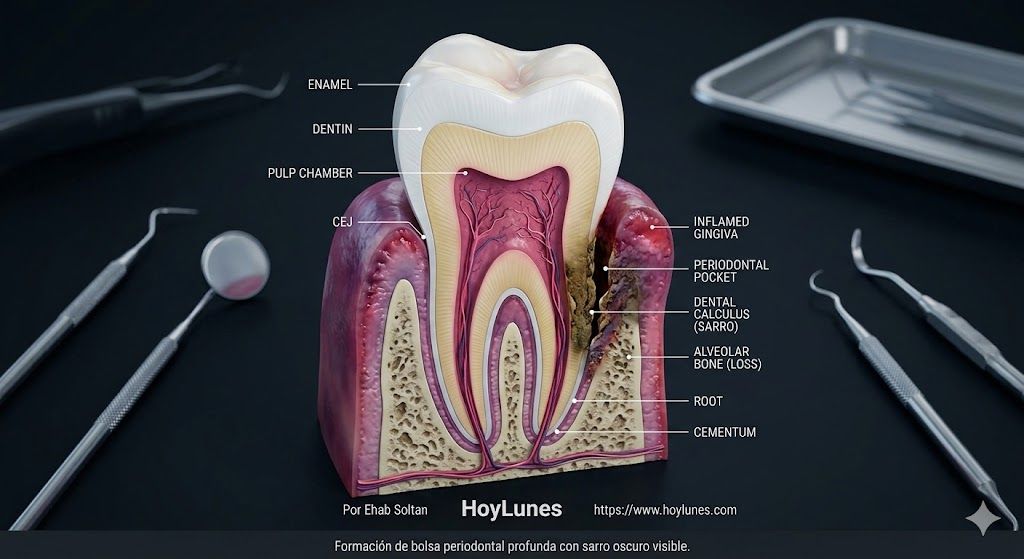
The Chronology of Collapse: How Long Does It Take for a Pillar to Fall?
David asked what we would all ask: “How could this happen to me overnight?” Dr. Arrieta’s response was blunt: it didn’t happen overnight.
Although the speed depends on factors like smoking and genetics, in a patient with uncontrolled diabetes, the clock runs faster:
Silence Phase (Gingivitis): The gums bleed but do not hurt. The patient ignores it.
Active Erosion: Diabetes alters the micro-blood vessels, preventing tissues from repairing themselves. The alveolar bone can be reabsorbed at a rate of 1 to 2 millimeters per year.
The Point of No Return: Once bone loss exceeds 70% of the root length, the tooth loses its mechanical stability. That is when a soft food becomes the “last straw” that topples the pillar.
“Maintaining a root remnant in a patient with metabolic risk is like leaving a window open in the middle of a storm: it is the gateway for systemic complications”.
David’s Verdict: A Rescue Surgery
Upon review, Dr. Arrieta discovered that David still had an infected root remnant in an adjacent area. His recommendation was drastic but necessary: immediate surgical extraction.
“In a patient with your cardiovascular profile, David, leaving that root there is like sleeping with a live grenade in your mouth”, the doctor explained.
The Action Plan
Sanitation Phase: Deep cleaning (curettage) to halt the release of pro-inflammatory cytokines that trigger insulin resistance.
Cardiovascular Prophylaxis: The risk of bacterial endocarditis was evaluated to decide on the use of pre-surgical antibiotics, following strict American Heart Association protocols.
Metabolic Rehabilitation: There will be no implants until David demonstrates stable glycemic control (HbA1c). Placing an implant in “diabetic” bone without control is condemning it to failure.
Real-World Recommendations
Dr. Arrieta praised David’s decision not to ignore the gap left by his molar. These are the shock measures that David—and anyone in his situation—must adopt:
Monitor Dry Mouth (Xerostomia): Many blood pressure medications reduce saliva, which is the natural protector against cavities. Hydration is not just about renal health; it is dental health.
The Sugar Myth: It is not just the quantity that matters, but the “stickiness” .Refined carbohydrates that adhere to the teeth fuel systemic inflammation.
The High-Risk Patient Schedule: Forget the annual check-up. A diabetic patient needs professional monitoring every 3 to 4 months.
The Tooth as a Messenger
The loss of a tooth without pain is not a random event; it is a symptom that the balance between the body and bacteria has been broken. As the American Academy of Periodontology indicates, there is a two-way street between the mouth and the rest of the body: what happens in your gums affects your pancreas and your arteries, and vice versa.
David did not return to the dentist just to regain his smile; he returned to regain control of his life. Because sometimes, the body’s silence is the loudest scream we can hear.
Consulted Sources
Journal of Periodontology (AAP)
American Heart Association (AHA) – Scientific Statements on Oral Health
FDI World Dental Federation – Oral Health and Diabetes
National Institute of Dental and Craniofacial Research (NIDCR)
Informative Note: This article is for informational and educational purposes only. The information presented here does not constitute a medical diagnosis nor does it replace, under any circumstances, the evaluation, advice, or treatment of a qualified dentist or physician. In the event of any tooth loss or symptoms of inflammation, it is imperative to seek professional consultation immediately to assess your general health status.
#OralHealth #Periodontitis #Diabetes #CardiovascularHealth #Prevention #Dentistry #ChronicInflammation #HoyLunes #EhabSoltan