Most damage does not begin with visible conflicts, but with the constant adaptation to tensions that the body registers as a threat. This article explores how the normalization of certain social dynamics can translate, over time, into real alterations of the cardiovascular system.
By Ehab Soltan
HoyLunes — There was no shouting. No one slammed the door. Everything unfolded within absolute normality.
In fact, if someone were to ask you, you would say you are fine. But as you hang up the phone or walk away from that person, you feel a weight at the base of your neck that wasn’t there ten minutes ago. It is a fatigue that does not improve with sleep, because it is not born of effort, but of constant vigilance.
This is the point where most people make a calculation error: believing that if there is no explicit conflict, there is no damage.
The Fallacy of Intensity
Our culture has trained us to identify danger in seismic events: the firing, the divorce, the loss. However, research in health and neuroscience suggests that the true risk to cardiovascular and metabolic health does not reside in the isolated event, but in the chronic exposure to low-intensity stressors.
What you call “managing a relationship”, your biology registers as a burden.
Allostasis is the body’s ability to achieve stability through change. When you interact in an environment where you must measure your words, predict the other person’s mood, or inhibit your responses to maintain peace, your brain activates the hypothalamic-pituitary-adrenal (HPA) axis. It does not do so because there is a death threat, but because the cost of the interaction is high.
The problem is that you have mentally accustomed yourself to this cost, but your endothelium has not.

From Social Tension to Arterial Lesion
When this activation becomes the basal tone of your day-to-day life, the stress response stops being a survival mechanism and becomes an erosive agent. This is not a guess; it is a documented sequence of physiological events:
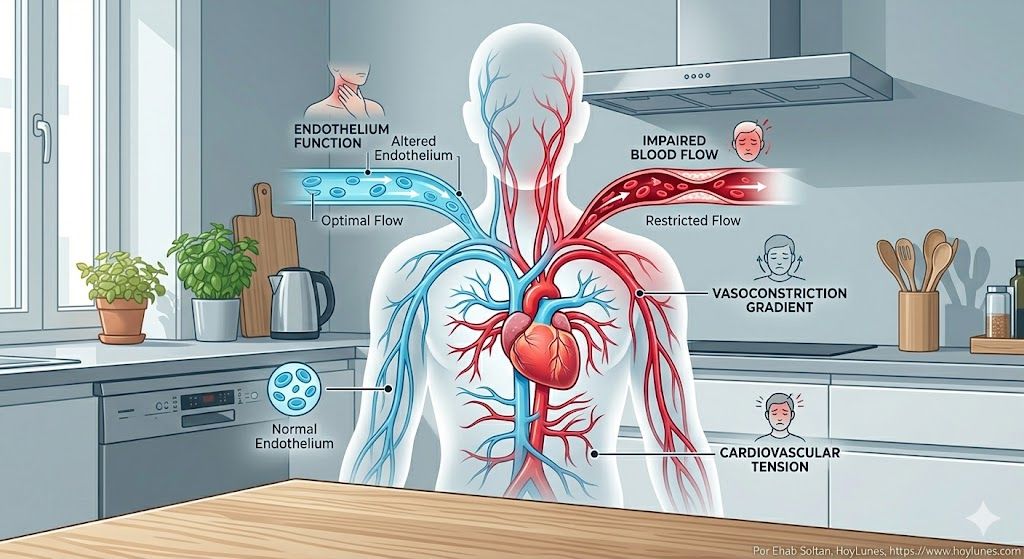
Vigilance and Vasoconstriction: The constant need to anticipate others’ reactions keeps the sympathetic tone elevated, which can favor sustained peripheral vasoconstriction.
Endothelial Damage: Studies published in journals such as Psychosomatic Medicine have shown that chronic social stress impairs endothelial function (the ability of your arteries to dilate). A rigid endothelium is the prelude to arterial hypertension.
Low-Grade Inflammation: Constant exposure to cortisol—the stress hormone—eventually generates resistance in the glucocorticoid receptors. The result is that the body loses the ability to put the brakes on inflammation, favoring a state of low-grade inflammation that can, over time, affect various systems of the organism.
The Risk of Adaptation
The most dangerous part of your situation is not the discomfort, but your ability to normalize it.
The human brain has an amazing plasticity for integrating unease as part of the landscape. You can spend years justifying an exhausting dynamic as “the other person’s character” or “the demands of the job”, until your body stops adapting.
Low heart rate variability (HRV) is associated with a lower recovery capacity of the nervous system. You are living in a state of permanent alert that consumes biological resources originally intended for cellular repair and immune defense.
When Data Contradicts Intuition
Massive investigations, such as the INTERHEART study conducted in 52 countries, have identified that psychosocial factors (including sustained tension at home or at work) can have a weight in the risk of myocardial infarction comparable to that of hypertension or obesity.
It is not a metaphor. It is a real statistical variable.
The body does not have a category for “inevitable social commitments.” For your cells, these situations can activate mechanisms similar to those of a perceived physical threat. The difference is that an acute threat ends in ten minutes, while a dysfunctional relationship can last decades.

The Shift in Perspective
If you have made it this far, you have probably already put a name and a face to that source of exhaustion. The conclusion should not be a “I need to try harder to be well.” In fact, the effort is what is making you sick.
Real health begins when you stop trying to “manage” the unsustainable and start recognizing the damage before it turns into an atheromatous plaque or an autoimmune disease.
This does not necessarily imply isolating oneself or breaking bonds. Isolation also has a proven biological cost. The difference is not in the presence or absence of relationships, but in the type of adaptation they demand. Health is not built by avoiding others, but by ceasing to sustain dynamics that force the body to remain in an uninterrupted state of alert.
The final question is not whether that relationship is “toxic” or not. The question is:
How much longer are you going to ask your body to sustain a peace that you do not feel?
#Neuroscience #CardiovascularHealth #ChronicStress #AllostaticLoad #HoyLunes #EhabSoltan



